|
More than 10% of caregivers look after a family member or friend from a distance. Not being nearby can make the task much more difficult and expensive. According to the latest AARP study, three-quarters of the family caregivers surveyed reported spending an average of $7,242 annually on out-of-pocket costs related to caregiving,. Long-distance caregivers often spend quite a bit more since long-distance caregivers are more likely than local caregivers to hire help, take unpaid time off work and pay for travel expenses.
The following tips can help make long-distance caregiving easier and more effective. Build a Team If you can’t physically check in on your loved one regularly, get help from others who can. This could be other family members or friends who live nearby, or even a friendly neighbor. Enlisting other family members can help lighten the load. They can pitch in to make daily check-in calls or handle tasks such as paying bills, making medical appointments and picking up groceries. If you have the resources, consider hiring a Certified Senior Advisor to help you evaluate your loved one’s care needs or hire home care aides if necessary. A certified Senior Advisor will have extensive experience in the senior care industry. An initial consultation up to one hour is typically free of charge, but then the advisor can be enlisted as necessary on an hourly basis. For instance, if there is an emergency and you need a trusted advisor to make a hospital visit, they can step in and keep you up to date. In home care aides can be in the home 24/7 which is nice for peace of mind but with hourly fees ranging from $30-50 per hour in can become expensive very quickly. Utilize Technology Devices like an iPhone or an Alexa can make video calls easy but those aren’t the only tools that can make help long-distance caregivers. Medical alert systems can allow a loved one to summon aid, and some have fall detection technology that will alert emergency responders even if your loved one is unable to communicate that they need help. Smart medication dispensers manage medications and let caregivers know if doses aren’t taken. Smart home systems can also help. A smart door lock, for example, can allow you to grant access to someone such as a friend or a health aide. Smart light bulb can allow your loved one to turn lights on or off with just the sound of their voice and a smart thermostat can help you ensure a comfortable temperature. Research Available Resources Your loved one may be eligible for public benefits that could help with caregiving tasks or costs. Start your search at Benefits.gov. Veterans often have many resources available to them, but the system can be difficult to navigate. Elder Veterans Legal Aid Group is and excellent resource to help guide you in the right direction. Be sure to ask about other resources, such as long-term care insurance. In the event that assisted living is necessary you may need to look at utilizing savings or home equity. Talking about money can be difficult, but the sooner you have the conversation the easier it will be to navigate a crisis should one arise. An Elder Law Attorney or a Certified Senior Advisor can be instrumental in guiding these conversations. This estate planning workbook can be helpful when planning for care, finances and end of life if arrangements have not already been made. Having a plan in writing can provide a lot of peace of mind. Forgetting things occasionally is a part of life. It's why individuals may have alerts on their smartphones or notes on their refrigerators. As people get older they might experience more frequent instances of forgetfulness, however this is often nothing to be concerned about. So how can seniors tell if they're experiencing the signs of dementia and when it's time to tell a doctor? Here are some pointers on hot to distinguish typical forgetfulness from dementia.
Typical age-related signs: Transience and absentmindedness Harvard Medical School stated that these two conditions are a regular part of the aging process. Transience is when the brain forgets some memories over time. According to the school, this could in fact be a good thing, due to the fact that it implies the brain is removing unused memories to include new ones. Absentmindedness is similar because it associates with your brain's focus. For example, forgetting an appointment might occur merely due to the fact that you weren't preoccupied with the idea of it. Lapse of memory and other mental issues According to the National Institute on Aging, there are lots of other health conditions that could contribute to memory loss. For instance, people with anxiety are often mistaken for having the symptoms of dementia. One reason for this might be that a person handling anxiety may be very preoccupied with the reason for their unhappiness and stress and anxiety. Constantly stressing over or obsessing over a current problem can result in lapse of memory of other subjects. Possible indications of dementia: Amnesia Unlike typical age-related lapse of memory, amnesia connected to dementia is progressive, according to Dr. William W. Pendlebury, a teacher at the University of Vermont. These issues get progressively worse and the client may ultimately need to relocate to a memory care community due to the fact that he can no longer reside on his own. Forgetting important details The symptoms of dementia go beyond merely forgetting where an object was positioned or when a visit was arranged. Pendlebury even more stated that symptoms consist of forgetting names of friends and loved ones and an inability to keep in mind some words. When an older adult shows these indications of severe lapse of memory, it's time to consider scheduling a visit the physician. Personality modification According to the Alzheimer's Association, individuals with dementia may experience significant changes in personality. For example, a senior experiencing dementia might suddenly be more prone to aggressive habits, paranoia or impulsiveness. Typically, this is the hardest part of the disease for caretakers to handle. The association stated that it is regular for senior caregivers to feel stressed out by these signs. As such, it could be smart to consider utilizing respite care services if it ends up being overwhelming. Disorientation Another typical symptom of dementia is the tendency to become disoriented in new environments. The University of Illinois said that this disorientation extends to both place and time. If an older adult with dementia relocate to a new place, the unknown stimuli might cause a feeling of insecurity. When disoriented, seniors with dementia may appear lost to onlookers and become quickly aggravated with their caregivers. Age-related memory loss and dementia are extremely different conditions, though they might share some overlap in signs. However, normal lapse of memory is frequently brought on by absence of focus and it never advances into serious area. Dementia, on the other hand, will become worse over time. If you have doubt about your signs, arrange a visit with your physician. As the weather turns colder here in Spokane it is important to make sure our seniors are staying warm and safe. Older adults can lose body heat faster than when they were young. A big chill can turn into a dangerous problem before an older person even knows what's happening. Beware of Hypothermia Hypothermia is caused by prolonged exposures to very cold temperatures. When exposed to cold temperatures, your body begins to lose heat faster than it’s produced. For an older person, a body temperature of 95°F or lower can cause many health problems. Low Body temperature affects the brain, making the victim unable to think clearly or move well. This makes hypothermia especially dangerous, because a person may not know that it’s happening and won’t be able to do anything about it. Keep Warm Inside Living in a cold house or apartment can cause hypothermia. Do not let it get too cold inside and dress warmly. Even if you keep your temperature between 60°F and 65°F, your home may not be warm enough to keep you safe. Here are some tips for keeping warm while you're inside:
Keep Warm Outside Check the weather forecast for cold and windy days. If you have to go out, wear warm clothes, and don't stay out in the cold and wind for a long time.
Some illnesses may make it harder for your body to stay warm.
What Are the Warning Signs of Hypothermia? Sometimes it is hard to tell if a person has hypothermia. Look for clues. Is the house very cold? Is the person not dressed for cold weather? Is the person speaking slower than normal and having trouble keeping his or her balance? Watch for the signs of hypothermia in yourself, too. You might become confused if your body temperature gets very low. Talk to your family and friends about the warning signs so they can look out for you. Early signs of hypothermia:
Later signs of hypothermia:
Call 9-1-1 right away if you think someone has warning signs of hypothermia. What to do after you call 9-1-1:
It is a sad fact that approximately one third of people over the age of 65 fall once or more per year. As many as 50% of these falls result in some form of injury. This includes cuts, bruises, fractures, head trauma and even death. On top of the physical harm caused by falls, they can also result in a loss of confidence and have serious long term emotional and psychological consequences. For many a fall can end up being a life changing event. It is estimated that 40% of admissions to assisted living communities are at least partly due to a fall at home.
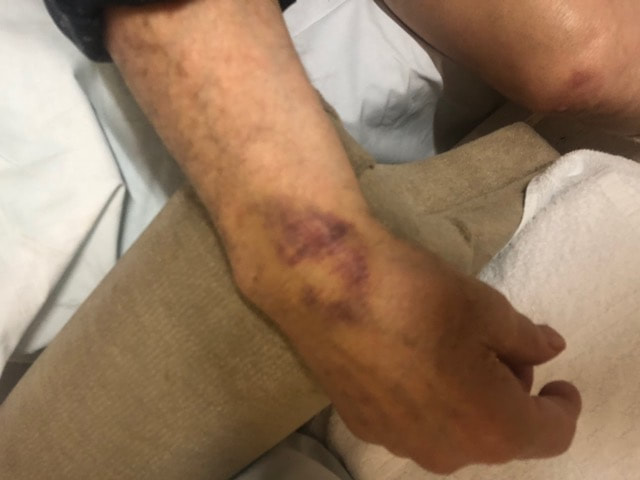
One of the most underestimated consequences of a fall is the effect it can have on an elderly person’s confidence. For someone that has lived independently their whole life a fall can be a very frightening experience, particularly if it results in even a minor injury, or an extended period of time unable to get themselves up off of the floor. This fear can result in an understandable reluctance to avoid situations which could potentially result in further falls. This tends to manifest itself as a withdrawal from social and physical activities, with the elderly person becoming increasingly sedentary and homebound. A reduction in physical activity has a direct impact on health and fitness leading towards frailty and an increased chance of further falls. This is further compounded by the poorer diet that can result from an unwillingness to risk falls while shopping or cooking. Spending the majority of their time alone at home can also have a significant impact on mental health. As we age our reactions tend to slow, with elderly people often failing to break their fall and being unable to control how they impact the ground, floor or furniture. This can be especially dangerous in high risk areas such as the kitchen or bathroom. Fractures are a serious risk, with those to the wrist and hip being the most common. Recovery time from such breaks is higher among the elderly and often involves extended hospitalization. Hip fractures are particularly dangerous, with one in twenty of those who suffer such an injury dying in the hospital and the mortality rate rising up to one third after twelve months. Treatment often involves long hospital stays, which contribute to muscle wasting and a difficulty returning to pre-injury fitness levels. Those who recover often still suffer from long term consequences, with most struggling to climb stairs and many being unable to get out of bed unassisted. Overall, falls are the main cause of accidental death in older people. After the fall itself, elderly people often find themselves unable to get up unassisted. An extended period of time on the floor can exacerbate any injuries caused by a fall. Response time is very important, timely medical care reduces the chance for further complications and reduces the length of hospital stays. Even when no injury is caused by the fall itself, the period of time on the floor can cause harm. Dehydration is a real risk, particularly if the elderly person exerts themselves struggling to get up. These physical dangers are matched by the psychological and emotional harm that can be caused by being left helpless on the floor. A wait of hours can be a very traumatic experience, especially if in the elderly person is in pain and unsure of when help will arrive. Some falls are caused by unsteadiness or slow reactions, but many can be the result of underlying medical conditions or serious events such as heart attacks or strokes. There are a number of such serious medical problems that can require immediate intervention or treatment. If the elderly person is unable to call for help or reach a telephone a treatable problem could become far more serious and potentially even fatal. Ensuring that help is available as soon as possible is crucial to minimizing the negative consequences of a fall in the home. Emergency Alert Pendants are particularly effective at providing help in a timely manner. They can be activated by the push of a button in the event of an accident and some even have automatic fall detection. This will contact an Emergency Response Center where an operator will be able to speak to the wearer and send help if needed. The reassurance of a friendly voice immediately after a fall can be as important as the help being dispatched. The elderly person has no need to panic or risk further injury struggling to get up and does not have to worry. Knowing that this protection is in place enables the wearer to live an independent life in their own home without the fear of being stranded after a fall. Many wearers of Emergency Alert Pendants report having the confidence to remain independent in their homes and family members report greater peace of mind knowing help is available at the push of a button. Most physical wounds heal in time. But elder abuse can cause harm to physical and psychological health, destroy social and family ties, lead to devastating financial loss, and more. Any type of mistreatment can leave the abused person feeling fearful and depressed. Sometimes, the victim thinks the abuse is his or her fault.
The most common forms of elder abuse Physical abuse happens when someone causes bodily harm by hitting, pushing, or slapping. This may also include restraining an older adult against their will, such as locking them in a room or tying them to furniture. Emotional abuse, sometimes called psychological abuse, can include a caregiver saying hurtful words, yelling, threatening, or repeatedly ignoring the older adult. Keeping that person from seeing close friends and relatives is another form of emotional abuse. Neglect occurs when the caregiver does not try to respond to the older adult's needs. This may include physical, emotional, and social needs, or withholding food, medications, or access to health care. Abandonment is leaving an older adult who needs help alone without planning for his or her care. Sexual abuse involves a caregiver forcing an older adult to watch or be part of sexual acts. Financial abuse happens when money or belongings are stolen from an older adult. It can include forging checks, taking someone else's retirement or Social Security benefits, or using a person's credit cards and bank accounts without their permission. It also includes changing names on a will, bank account, life insurance policy, or title to a house without permission. Recognizing the signs of elder abuse.
In most states doctors, lawyers and professional caregivers are mandatory reporters in cases of elder abuse. Family and friends can also report it. Do not wait. Help is available. If you think someone is in urgent danger, call 911 or your local police to get help right away. We all age differently so, there is no way to set one age when everyone should stop driving. Trouble seeing, trouble hearing, slower reaction time and certain medications can all effect a person’s ability to drive safely. As you age it may become harder to see people, and movement outside your direct line of sight. At night, you may have trouble seeing things clearly. Glare from oncoming headlights or street lights can be a problem. Eye conditions, such as glaucoma, cataracts, and macular degeneration, can also cause interfere with your ability to drive confidently. Aging may affect your hearing as well, making it harder to notice horns, sirens, or even noises coming from your own car. This can be a problem because these sounds warn you when you may need to pull over or get out of the way. Many medications have side effects that can make driving unsafe. Some may even come with warnings about driving while taking them. Pay attention to how these drugs may affect your driving and never drive if you feel drowsy or lightheaded. Safe driving tips for seniors:
Sometimes, it can be hard for an older person to realize that he or she is no longer a safe driver. If possible, try to observe the person’s driving in person. If it’s not possible to observe the older person driving, look for these signs:
Talking with a senior about their driving. For many people, driving represents independence, so giving up that freedom can be extremely difficult. Avoid a confrontation or an intervention with the entire family. You may want to be the one who has the conversation with your aging parent or elderly relative about their driving, however, consider that your loved one may be more open to listening to someone else. When choosing who will initiate the conversation with your older family member about his or her driving, consider the relationships and personalities involved. Try to keep the conversation one-on-one and pick a time of day when you believe your loved one will be most relaxed. Let your loved one know that your goal is to make sure they’re safe and that you wish for them to remain independent and will do all you can to help. Avoid saying they are a dangerous driver and starting out the conversation by demanding they need to stop driving. Focus on the facts available to you, such as their medical condition or your first-hand experience of their unsafe driving. If your aging relative wishes to remain independent, then an alternative means of transportation will be necessary.
Safe Driving Self Assessment Questions:
If you answered “yes” to any of these questions, it may be time to talk with your doctor about driving or have a driving assessment. Everyone feels tired now and then. But, If you continue to feel tired for weeks in a row, it's time to see your doctor. They may be able to help you find out what's causing your fatigue. In fact, your doctor may even suggest you become more active, as exercise may reduce fatigue and improve quality of life.
Sometimes, fatigue can be the first sign that something is wrong in your body. For example, people with COPD, often complain of fatigue. People with cancer may feel fatigued from the disease, the treatments, or both. Fatigue can be attributed to many medical conditions including:
Emotional stresses can take a toll on your energy. Fatigue can be linked to many conditions, including:
Some lifestyle habits can add to fatigue:
How can I feel less fatigued? Some changes to your lifestyle can make you feel less tired:
When should I see a doctor for fatigue? If you've been tired for several weeks with no relief, it may be time to call your healthcare provider. He or she will ask questions about your sleep, daily activities, appetite, and exercise and will likely give you a physical exam and order lab tests. Your treatment will be based on your history and the results of your exam. Your doctor may prescribe medications to target underlying health problems. Medicare Supplement Insurance, often referred to as Medigap, is insurance that helps fill "gaps” in Original Medicare insurance and is sold by private companies. Original Medicare pays a significant portion of the cost for covered health care services and supplies but not the full cost. A Medicare Supplement Insurance policy (Medigap) can help pay some of the remaining health care costs such as copayments, coinsurance, and deductibles.
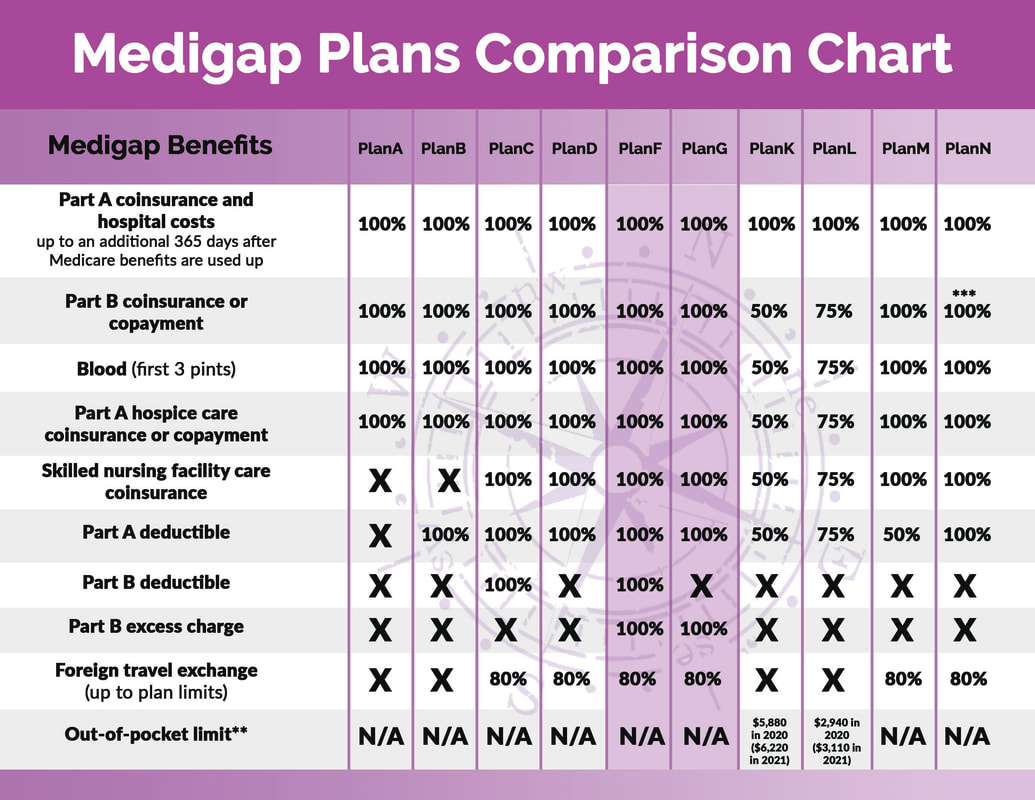
There are significant overlaps between many of the plans so you may find the chart below helpful to compare and contrast your options. * Plans F and G also offer a high-deductible plan in some states. With this option, you must pay for Medicare-covered costs (coinsurance, copayments, and deductibles) up to the deductible amount of $2,340 in 2020 ($2,370 in 2021) before your policy pays anything. (Plans C and F aren't available to people who were newly eligible for Medicare on or after January 1, 2020.)
** For Plans K and L, after you meet your out-of-pocket yearly limit and your yearly Part B deductible, the Medigap plan pays 100% of covered services for the rest of the calendar year. *** Plan N pays 100% of the Part B coinsurance, except for a copayment of up to $20 for some office visits and up to a $50 copayment for emergency room visits that don't result in inpatient admission. Medicare Supplement Plan A: Medicare Supplement insurance Plan A is different from Medicare Part A, although their similar names may be confusingly similar. Medicare Part A covers inpatient hospital care and is one half of Medicare (Part A and Part B). Medicare Supplement insurance Plan A provides coverage that helps pay for out-of-pocket costs from Medicare Part A and Part B. Medicare Supplement Plan B: Medicare Supplemental insurance Plan B is different from Medicare Part B, although their similar names may be confusingly similar. Medicare Supplemental Plan B covers
Medicare Supplement Plan C covers:
Medicare Supplement Plan D Covers:
Medicare Supplement Plan F covers:
Medicare Supplement Plan G covers:
Medicare Supplement Plan K covers:
Medicare Supplement Plan L covers: 100% of the cost of:
Medicare Supplement Plan M covers:
Medicare Supplement Plan N covers:
When someone you love dies, the job of handling the personal and legal details may feel overwhelming during a time of grief. It is a big responsibility that can take a year or more to complete. It is unlikely you will be able to do it alone. Settling a deceased family member's affairs is not a one-person task. You may need the help of others, ranging from lawyers and CPA’s to funeral directors and movers. Also don’t be afraid to ask for help from trusted friends and relatives. Making a list details that need to be addressed will help keep you organized and prevent things from slipping through the cracks. This guide will get you started. 1. Get a legal pronouncement of death As soon as possible, the death must be officially pronounced by someone in authority like a doctor in a hospital or nursing facility or a hospice nurse. This person also fills out the forms certifying the cause, time, and place of death. These steps will make it possible for an official death certificate to be prepared. This legal form is necessary for many reasons, including life insurance and property issues. 2. Arrange for transportation of the body Arrangements should be made to pick up the body as soon as the family is ready and according to local laws. This can be done by a funeral home or by the family themselves in most states. If the death takes place in a hospital or nursing facility, they may help with these arrangements. If at home, you will need to contact a funeral home directly. 3. Notify family and friends How to notify friends and family is a personal choice. You may choose to send out a group text or mass email or make individual phone calls to let people know their loved one has died. Ask the recipients to spread the word by notifying others connected to the deceased. 4. Locate Important Papers Find the deceased’s important papers and documents as soon as possible. If necessary, ask close family, friends, or the deceased's doctor or lawyer if they know where these important papers can be found, and the location of a bank safety deposit box, if any. You will want to seek out the Will, insurance policies, titles, deeds, trusts, bank accounts, power of attorney etc. 5. Arrange for care of dependents If the deceased has dependent children or perhaps is the primary care giver for a spouse or other family member it will be necessary to make arrangements for the care of the dependent. This care can look very different depending on the age, health and mental capacity of the dependent. Initially it may be easiest for a family member to fill the role while a long-term plan is developed. If plans are not made in advance and you need to research options, the Department of Social and Health Services may be a good place to start. 6. Arrange for care of pets When selecting a caregiver for pets, consider partners, adult children, parents, brothers, sisters, and friends who have met your pet and have successfully cared for pets themselves. Remember, the new owner will have full discretion over the animal’s care including veterinary treatment and euthanasia. If there is no one available to take the pet it may be necessary to contact a local animal shelter. 7. Contact person’s employer Contact the deceased’s employer and ask about any possible death benefits, retirement annuity or pension plans, and life and health insurance coverage. Unions and other professional organizations may provide benefits also. Sometimes you may need to return the deceased’s final monthly pension payment to the pension company before they send a new, adjusted payment. 8. Arrange for funeral Planning a funeral or memorial service is a highly personal process. Your decisions will be shaped by your life experiences, relationship to the deceased, what the deceased wanted, religious beliefs, and myriad other factors. 9. Arrange to look after persons home and collect mail To forward the persons mail to yourself at a different address you will need to file a request at your local post office. Bring proof that you are the executor or administrator authorized to manage the deceased’s mail then fill out a forwarding change of address form. 10. Make sure important bills continue to be paid Unpaid debt becomes the responsibility of the deceased person’s estate. The trustee responsible for overseeing the estate first will use any assets in the estate to pay creditors before dividing the assets among the heirs according to the deceased’s will, if there is one. This process is called probate. Making sure property taxes, mortgage payments and certain utilities remain current will help you avoid complications down the road. Also be sure to cancel services that may no longer be needed such as phone and television. 11. Get multiple copies of death certificate In order to close many accounts, the companies involved will likely want a copy of the death certificate, especially when financial assets are involved. To order copies of a death certificate, contact the county or state vital records office in the place where the death occurred. They will tell you exactly what you need to do. In Washington state you can find the Information on the Department of Health website. 12. Additional contacts you may want to make:
People with Alzheimer’s and related dementias experience changes in thinking, remembering, and reasoning that affects nearly every aspect of daily life. Eventually people with Alzheimer’s will need assistance completing everyday tasks including dressing, bathing, and grooming. Often times It can be upsetting to the person to need help with such personal activities. Here are a few tips to consider as a caregiver to best help your loved one as the disease progresses:
Communication Tips to Help Care for People with Alzheimer’s Communication can become difficult for people with Alzheimer’s because they have trouble remembering things. This can lead to agitation or even anger. It is common for a person with Alzheimer’s to have trouble finding the right words. As a caregiver it is easy to feel frustrated or impatient, but it is important to understand that the disease is causing the change in communication skills.
Maintaining a Healthy and Active Lifestyle for People with Alzheimer’s Eating healthy and staying active is good for everyone. As the disease progresses, maintaining a healthy diet and staying active may be increasingly challenging.
Home Safety Tips for People With Alzheimer's As a caregiver or family member of a person with Alzheimer’s there are many things to consider that can make the home a safer place. Removing hazards and adding safety features around the home can help give the person more freedom to move around independently and safely.
You can download a Free Alzheimer’s home safety checklist. |
AuthorTyice Strahl Categories
All
Archives
May 2023
|
- Home
-
Settings
- Assisted Living
- Home Care
- Independent Living
- Memory Care
- Skilled Nursing
- Adult Family Homes
-
All Communities
>
- Aspen Quality Care
- Avamere South Hill
- Brighton Court
- Brookdale Nine Mile
- Brookdale Park Place
- Cheney Assisted Living
- Cherrywood Assisted Living
- Colonial Court
- Cornerstone Court
- Evergreen Fountains
- Palouse Country
- Fairview Assisted Living
- Fairwinds
- Fairwood
- Fieldstone Memory Care
- Good Samaritan
- Maplewood Gardens
- Moran Vista
- North Point Village
- Orchard Crest
- Pine Ridge Memory Care
- Emilie Court
- Ridgeview Place
- Riverview Retirement
- Rockwood Retirement Community
- Rose Pointe Assisted Living
- Royal Park
- South Hill Village
- Sullivan Park Assisted Living
- Sunshine Health Facilities
- Touchmark Assisted Living
- Willow Grove
- Wind River
- Alderwood Manor
- Franklin Hills
- Manor Care
- North Central Care Center
- Providence St Joseph
- Regency at Northpointe
- Royal Park Health and Rehabilitation
- Spokane Veterans Home
- The Gardens on University
- Spokane Assisted Living Directory
- Locations
- Services
- About
- Senior Living Blog
- Contact










 RSS Feed
RSS Feed
